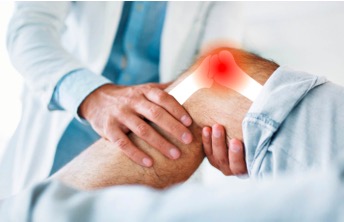
OA is diagnosed by a triad of typical symptoms, physical findings, and radiographic changes. The American College of Rheumatology has set forth classification criteria to aid in the identification of patients with symptomatic OA that include, but do not rely solely on, radiographic findings. Diagnosis of Osteoarthritis is done by noting the signs and symptoms:
- Pain on movement
- Chronic pain that gets worse over time
- Joint stiffness
- Tenderness around the joint
- A clicking or grinding sensation
- Crunching and creaking on movement
- Hard swelling around the joint
- Fluid swelling in the joint
- Limited range of movement
- Abnormal movement and joint laxity
- Loss of muscle size and strength

Impact of OA on Quality of Life
There are several ways in which OA can impact the quality of life such as increasing stress and sleep disruption due to pain that has intensified. Osteoarthritis also reduces the ability to perform normal activities in our daily life and reduces productivity. It can also lead to problems with anxiety and depression.
Pain and stiffness can decrease your desire to be active. Not only does a lack of activity limit your enjoyment of life — it can also reduce muscle mass which leads to muscle tightness and a risk of falling and suffering from other injuries. Muscles are more prone to injury when it is tight or weak, and micro-tears lead to scarring of the muscles that can disrupt normal muscle function, therefore affecting the surrounding connective tissues.
Lack of activity can also lead to weight gain. Extra weight may exacerbate OA symptoms, and this may lead to an increased risk of getting other complications such as:
- Diabetes
- Hypertension
- Heart disease
Other complications that can arise from OA are:
- Bone spurs
- Gait disturbance
- Loss of flexibility and stability
- Stress fractures
- Bleeding or infection in the joint
- Bone death (osteonecrosis)

Prevention of Osteoarthritis
A number of factors may put a person at risk of developing OA. Making changes may not prevent the condition, but a person may be able to reduce their risk or keep OA from advancing.
The Arthritis Foundation suggest the following:
- Maintain a healthy weight: Excess weight puts extra pressure on the knees. Over time, this contributes to wearing down the cartilage. Extra fat can also cause the body to produce cytokines, a type of protein. This can lead to widespread inflammation, and it can change the way that cartilage cells work.

- Controlling blood sugar: High glucose levels can affect the structure and function of cartilage, and diabetes increases the risk of inflammation and cartilage loss.
- Exercising regularly: Moderate exercise can help the joints stay flexible, strengthen the muscles that support the knees, and reduce the risk of many health conditions. It may help to garden, walk, or swim for 30 minutes at a time, five times a week.


- Reduce the risk of injury: Cartilage that sustains damage from an injury is more likely to develop arthritis later. Reduce the risk of tripping in the home, wear shoes that fit well, and use protective gear while playing sports to prevent injury.
- Avoiding overuse: Some sports or professions involve repetitive motions of the knee joint, such as kneeling or squatting. People who regularly lift more than 55 pounds may have an increased risk of OA. Jobs that put people at risk may include laying carpets and unloading trucks or ships. Repetitive exercise can increase the risk of developing OA of the knee.
- Physical therapy: Strengthening of the muscles around the knee joint may help decrease the burden on the knee. Preventing atrophy of the muscles is an important part of maintaining functional use of the knee.
- Undergoing posture and bone alignment tests: Some sources suggest that these can affect a person’s risk of developing OA.
- Eating a healthful diet, getting enough sleep, managing stress, and staying active all contribute to better overall well-being and a decreased risk of health issues, including OA.

How Oxidative Stress can lead to Osteoarthritis?
Oxidative stress happens when there is an imbalance between the number of free radicals and antioxidants in our body. This is particularly harmful as it can lead to cell and tissue damage. Oxidative stress is considered a main causative factor in the pathogenesis of OA. Many pro-inflammatory mediators or free radicals are elevated in OA, including Reactive Oxygen Species (ROS), and Reactive Nitrogen Species (RNS).

Source: https://www.sciencedirect.com/science/article/pii/S0925443916000041
The excessive production of free radicals can harm cell functionality as it damages cellular lipids, proteins and DNA. Free radicals can give rise to cartilage apoptosis/ cell death, thus accelerating articular cartilage dysfunction and degeneration.

Oxidative stress is known to be detrimental to many cells and to occur during disease and with ageing. It has also been implicated in the development of OA. Although osteoarthritis has been traditionally classified as a non-inflammatory arthritis, however evidence has increasingly shown that inflammation occurs as cytokines and metalloproteinases are released into the joint. Inflammation get worse when more of these agents are released, especially when triggered by excessive free radicals. Inflammation in the cartilage and synovial leads to loss of joint structure and progressive damage to the cartilage, causing OA to become worse. Inflamed articular cartilage still remains a huge hurdle to treat due to the limited self-healing capacity of the cartilage which lacks nerves and blood supply.
How Hydrogen Therapy Can Help?
Hydrogen therapy is one of the newest and most effective treatments to manage arthritis due to its role as a therapeutic antioxidant. It is able to selectively neutralize free radicals in the affected area which reduces inflammation and prevents further damage to the joint, thereby slowing down the progression of OA. As hydrogen is the smallest molecule on earth, it is able to diffuse itself into the targeted cells without affecting the functions of other cells and organs.
Based on a research by Ding Li and Wan Chun Wang in the year of 2012, hydrogen is considered to be a selective antioxidant and can be used as a kind of therapeutic medical gas. This further reinforces the idea that hydrogen treatment can help to decrease the damage of cartilage caused by oxidative stress.
In Hi-Bliss Hydrogen therapy centre, we combine the therapeutic benefits of hydrogen therapy with osteopathic manual practices. Our certified physiotherapist will perform the Osteopathic Structural and Functional Examination on the lower limb area to find out the root cause of the pain by measuring the Range of Motion (ROM), Muscle Strength, Gait Analysis, Posture Alignment, Quality of Movement, Pain during Movement, Muscle Bulk and Tone. The hydrogen treatment aims to suppress inflammatory factors such as free radicals and slow down the progression of osteoarthritis.
By combining the Hydrogen with Osteopathic practices, we help our clients reduce pain in the joint, slow down the progression of OA and ultimately help them return to normal daily life. Hydrogen therapy is efficient in treating the inflamed joints caused by OA by repairing the internal cells in our body while our physiotherapy/osteopathic techniques helps to improve the external muscles caused by muscle imbalance. We will also educate clients about suitable stretching and strengthening exercise that aims to manage symptoms and improve joint function, flexibility and balance.
By reducing the number of OA symptoms, it will improve your ability to get around and increase your quality of life.
Learn more how Hi-Bliss Hydrogen Therapy can help slow down the progression of OA here : https://wordpress-851564-2937612.cloudwaysapps.com/treatment-services-osteoarthritis-therapy/
References:
- https://springloadedtechnology.com/guide-to-severe-knee-osteoarthritis/
- https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925
- https://www.healthline.com/health/osteoarthritis#osteoarthritis-symptoms
- Targeting oxidative stress to reduce osteoarthritis - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4730642/
- ROS/oxidative stress signaling in osteoarthritis - https://www.sciencedirect.com/science/article/pii/S0925443916000041