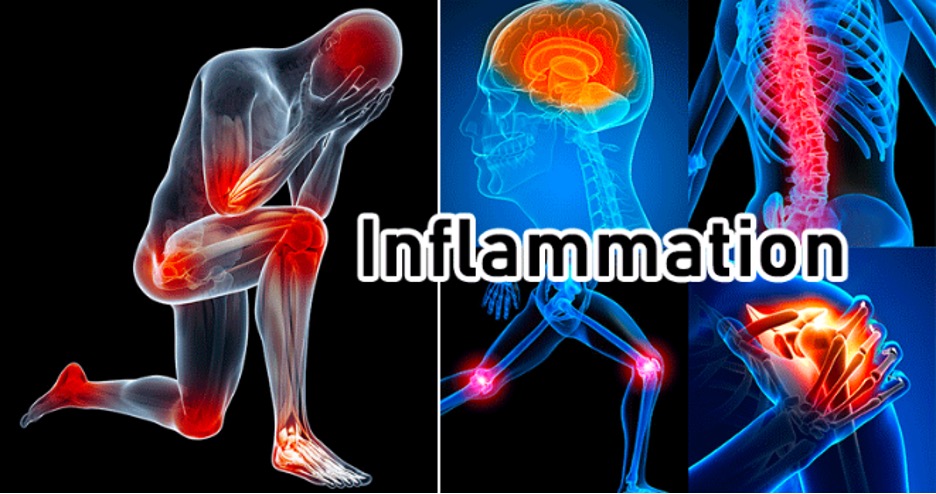
Based on visual observation, the ancients characterised inflammation by five cardinal signs, namely redness (rubor), swelling (tumour), heat (calor; only applicable to the body' extremities), pain (dolor) and loss of function (functio laesa).
More recently, inflammation was described as "the succession of changes which occurs in a living tissue when it is injured provided that the injury is not of such a degree as to at once destroy its structure and vitality", or "the reaction to injury of the living microcirculation and related tissues”.
The classical description of inflammation accounts for the visual changes seen. Thus, the sensation of heat is caused by the increased movement of blood through dilated vessels into the environmentally cooled extremities, also resulting on the increased redness (due to the additional number of erythrocytes passing through the area). The swelling (oedema) is the result of increased passage of fluid from dilated and permeable blood vessels into the surrounding tissues, infiltration of cells into the damaged area, and in prolonged inflammatory responses deposition of connective tissue.
Pain is due to the direct effects of mediators, either from initial damage or that resulting from the inflammatory response itself, and the stretching of sensory nerves due to oedema. The loss of function refers to either simple loss of mobility in a joint, due to the oedema and pain, or to the replacement of functional cells with scar tissue.
Today it is recognised that inflammation is far more complex than might first appear from the simple description given above and is a major response of the immune system to tissue damage and infection, although not all infection gives rise to inflammation. Inflammation is also diverse, ranging from the acute inflammation associated with S. aureus infection of the skin (the humble boil), through to chronic inflammatory processes resulting in remodeling of the artery wall in atherosclerosis; the bronchial wall in asthma and chronic bronchitis, and the debilitating destruction of the joints associated with rheumatoid arthritis .
In short, Inflammation is a vital part of the immune system's response to injury and infection. It is the body's way of signaling the immune system to heal and repair damaged tissue, as well as defend itself against foreign invaders, such as viruses and bacteria. Inflammation is considered the cornerstone of pathology in that the changes observed are indicative of injury and disease.
Without inflammation as a physiological response, wounds would fester, and infections could become deadly. However, if the inflammatory process goes on for too long or if the inflammatory response occurs in places where it is not needed, it can become problematic. Chronic inflammation has been linked to certain diseases such as heart disease or stroke, and may also lead to autoimmune disorders, such as rheumatoid arthritis and lupus.
Good Inflammation, Bad Inflammation: What are the different types of Inflammation?
There are 2 types of inflammation – the “Good” or protective type (which benefits health) and the “Bad” or harmful type (which destroys it).
- The Good: Acute (short-term) inflammation
An injury or illness can involve acute, or short-term, inflammation. Acute inflammation occurs after a cut on the knee, a sprained ankle or a sore throat. It is a short-term response with localized effects, meaning it works at the precise place where a problem exists. The telltale signs of acute inflammation include redness, swelling, heat and sometimes pain and loss of function, according to the National Library of Medicine.
These signs are not always present. Sometimes inflammation is “silent,” without symptoms. A person may also feel tired, generally unwell, and have a fever.
In the case of acute inflammation, blood vessels dilate, blood flow increases and white blood cells swarm the injured area to promote healing. This response is what causes the injured area to turn red and become swollen.
During acute inflammation, chemicals known as cytokines are released by the damaged tissue. The cytokines act as "emergency signals" that bring in your body's immune cells, hormones and nutrients to fix the problem.
In addition, hormone-like substances known as prostaglandins create blood clots to heal damaged tissue, and they also trigger pain and fever as part of the healing process. As the body heals, the acute inflammation gradually subsides.
Symptoms of acute inflammation last a few days. Subacute inflammation lasts 2–6 weeks.
- The Bad: Chronic (long-term) inflammation
Unlike acute inflammation, chronic inflammation can have long-term and whole-body effects. Chronic inflammation is also called persistent, low-grade inflammation because it produces a steady, low-level of inflammation throughout the body, as judged by a small rise in immune system markers found in blood or tissue. This type of systemic inflammation can contribute to the development of disease, according to a summary in the Johns Hopkins Health Review.
Low levels of inflammation can be triggered by a perceived internal threat, even when there isn't a disease to fight or an injury to heal, and sometimes this signals the immune system to respond. As a result, white blood cells swarm but have nothing to do and nowhere to go, and they may eventually start attacking internal organs or other healthy tissues and cells.
Researchers are still working to understand the implications of chronic inflammation on the body and the mechanisms involved in the process, but it's known to play a role in the development of many diseases.
Causes of Inflammation
Inflammation happens when a physical factor triggers an immune reaction. Inflammation does not necessarily mean that there is an infection, but an infection can cause inflammation.
Acute inflammation
Acute inflammation can result from:
- exposure to a substance, such as a bee sting or dust | an injury | an infection
When the body detects damage or pathogens, the immune system triggers a number of reactions:
- Tissues accumulate plasma proteins, leading to a buildup of fluid that results in swelling.
- The body releases neutrophils, a type of white blood cell, or leukocyte, which move toward the affected area. Leukocytes contain molecules that can help fight pathogens.
- Small blood vessels enlarge to enable leukocytes and plasma proteins to reach the injury site more easily.
Signs of acute inflammation can appear within hours or days, depending on the cause. In some cases, they can rapidly become severe. How they develop and how long they last will depend on the cause, which part of the body they affect, and individual factors.
Some factors and infections that can lead to acute inflammation include:
- acute bronchitis, appendicitis and other illnesses ending in “-itis”
- an ingrown toenail
- a sore throat from a cold or flu
- physical trauma or wound
Chronic Inflammation
Chronic inflammation can develop if a person has:
- Sensitivity: Inflammation happens when the body senses something that should not be there. Hypersensitivity to an external trigger can result in an allergy.
- Exposure: Sometimes, long-term, low-level exposure to an irritant, such as an industrial chemical, can result in chronic inflammation.
- Autoimmune disorders: The immune system mistakenly attacks normal healthy tissue, as in psoriasis.
- Autoinflammatory diseases: A genetic factor affects the way the immune system works, as in Behçet’s disease.
- Persistent acute inflammation: In some cases, a person may not fully recover from acute inflammation. Sometimes, this can lead to chronic inflammation.
Factors that may increase the risk of chronic inflammation include:
- older age | obesity | a diet that is rich in unhealthful fats and added sugar | smoking | low sex hormones | stress | sleep problems
Chronic inflammation can continue for months or years. It either has or may have links to various diseases, such as:
Diabetes | Cardiovascular disease (CVD) | Arthritis and other joint diseases | Allergies | Chronic obstructive pulmonary disease (COPD) | Psoriasis | Rheumatoid Arthritis
The symptoms will depend on the disease, but they may include pain and fatigue.

For example, chronic inflammation has been linked to heart disease and stroke. One theory suggests that when inflammatory cells stay too long in blood vessels, they promote the buildup of plaque. The body perceives this plaque as a foreign substance that doesn't belong, so it tries to wall off the plaque from the blood flowing inside the arteries, according to the American Heart Association (AHA). If the plaque becomes unstable and ruptures, it forms a clot that blocks blood flow to the heart or brain, triggering a heart attack or stroke.
Cancer is another disease linked with chronic inflammation. Over time, chronic inflammation can cause DNA damage and lead to some forms of cancer, according to the National Cancer Institute.
Chronic, low-grade inflammation often does not have symptoms, but doctors can test for C-reactive protein (CRP), a marker for inflammation in the blood. High levels of CRP have been linked with an increased risk of heart disease. CRP levels can also indicate an infection, or a chronic inflammatory disease, such as rheumatoid arthritis or lupus, according to the Mayo Clinic.
Besides looking for clues in the blood, a person's diet, lifestyle habits and environmental exposures can contribute to chronic inflammation. It is important to maintain a healthy lifestyle to keep inflammation in check.
The following table summarizes some key differences between acute and chronic inflammation:

Let’s look at Signs of you have Inflammation and more on Chronic Inflammation – The New Silent Killer in more depth in the next blog.
Learn more how Hi-Bliss Hydrogen Therapy can help reduce Inflammation here : https://wordpress-851564-2937612.cloudwaysapps.com/what-is-hibliss-hydrogen-therapy/
Sources:
- What is Inflammation?
https://www.livescience.com/52344-inflammation.html - Journal of Inflammation https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1074343/pdf/1476-9255-1-1.pdf